This ‘Smart Jacket’ Is Smart Enough To Save The Lives Of Children In Uganda And Beyond
Before Brian Turyabagye scribbled his name in the annals of African tech innovations with his groundbreaking invention; a biomedical smart jacket that accurately detects pneumonia, he was just another tech-savvy individual who liked to tinker with stuff.
His time at Uganda’s Makerere University – from where he obtained a Bachelor’s degree in Telecommunications Engineering back in 2015 – was quite eventful. The period of his studies was interspersed with stints at the Uganda Communications Commission where he interned, as well as iLabs@Mak; a technology lab at his alma mater.
It was, perhaps, the spell at the technology lab that whetted his appetite for tech. During that period, he worked on several projects which have technology at their core and was even saddled with the responsibility of running point on some of those.
By the time Turyabagye left iLabs@Mak, he had proved his worth on a smartphone project and weighed in significantly as Team Lead on a number of IT projects for both mobile and web-based systems. And it was always something of a given that he was to snap up his first job soon after graduating from college as IT Systems Officer at Uganda’s NC Bank.

Source: LinkedIn
But his appetite for tech was not going to be quelled even while on the corporate job. His interest in smart technologies like Machine Learning and Artificial Intelligence soon led him into founding his own tech company, SkyApps Technologies Limited, in July 2016.
Turybagye set up SkyApps as a software solutions company that is focused on developing advanced AI platforms and Android-based solutions. The idea was to keep his day job and run the tech firm as a side hustle; one borne out of his professional fascination and curiosity. But little did he know that he would be dabbling into yet another project just a few months on.
It was a couple of months after Turyabagye had gotten his small AI firm off the ground and some misfortune had arrived unannounced when a close friend and business partner, Olivia Koburongo, lost her grandmother in somewhat mitigable circumstances.
She’d been sick.
The ailment had taken the old woman to several clinics and at the end of every test, the same diagnosis, or perhaps, misdiagnosis, had come up.
Olivia’s grandmother was led to believe her health was failing because of Malaria, and maybe she’d still be alive if that were true.
All the anti-malarial medication that went into her treatment had little effect and when she eventually passed on, the prognosis reports indicated that she had actually been suffering from pneumonia. The misdiagnosis led to fatal consequences.
Although Olivia’s grandmother was aged, it broke hearts that she could have been around a while longer and her premature demise was caused by misleading information.
When Turyabagye learned of the circumstances surrounding the demise of his partner’s grandmother, he was disturbed by the dastardly effect of the misdiagnosis and the thought of losing lives to such scenarios may have tied his gut into a painful knot.

One cursory look into the matter and it dawned on him that pneumonia was actually a bigger problem than he had thought. And because it was not found out quickly enough or often misdiagnosed as malaria, it was, in fact, children who were bearing most of the brunt.
Data from UNICEF has it that pneumonia kills half a million children under five in sub-Saharan Africa each year. On a global level, the WHO brands it a “deadly condition” that is responsible for a disturbing 16 percent of all deaths of children under five. And slow diagnosis, or even misdiagnosis, is cited as one of the main reasons the ailment leaves so many bodies in its wake.
When Turyabagye relayed his findings to his then recently bereaved partner, as much concern was elicited and the duo soon got working on their knowledge of the medical condition. What followed was a series of consultations with medical experts on the specific symptoms of the ailment and by the time they had learned enough, it was time to work on a solution.
And what a solution it turned out to be. Because of his history, Turyabagye was always going to favour a tech solution. But this time though, it’d be the first time he’d actually be using technology to help save lives, or at least, prolong it.

Source: cnn.com
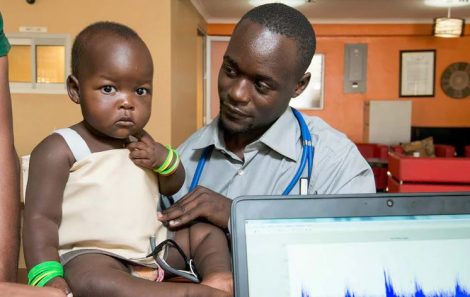
By leveraging the expertise of Mwikirize Cosmas; who was once his tutor at Makerere University, as well as inputs from medical and tech experts, Turyabagye and his team created Mama-Ope; a biomedical smart jacket that rapidly increases the accuracy and speed of diagnosing pneumonia.
The device is believed to diagnose the condition four-times faster than medical personnel, and with considerable accuracy. Once a patient is clad in the jacket, it analyzes the chest area and then transmits its findings via Bluetooth to a smartphone app.

The smart jacket works on a similar technology as the stethoscope. Once one is strapped in the jacket, it stretches across the chest and side of the person and examines specific points on the lungs for symptoms of pneumonia, which has swelling of the lungs as one of its more common features.
On completion of the examination, data is automatically sent via Bluetooth to a mobile app which records and analyses the information – aiding the healthcare professional in making an informed diagnosis.
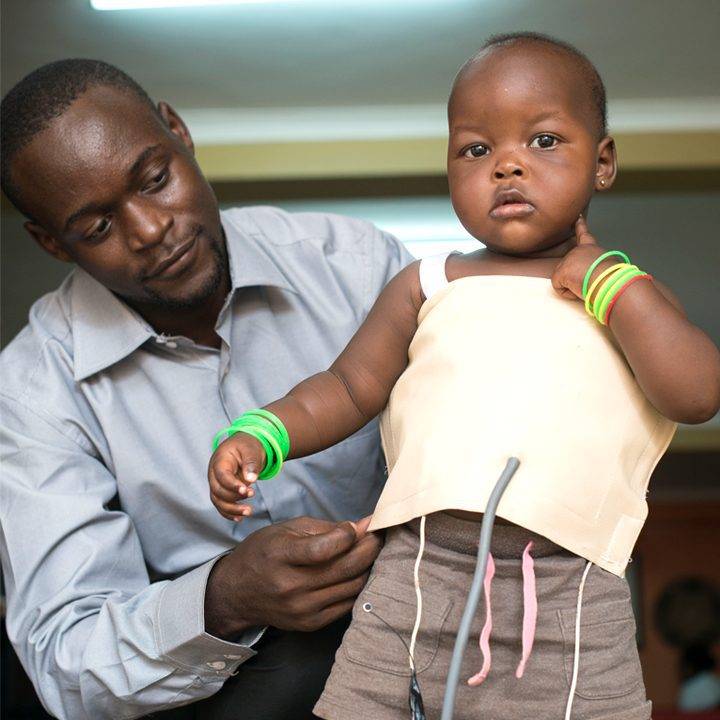
According to the Ugandan techie, the jacket reduces human error to an infinitesimal degree and provides accurate diagnosis up to four times faster than the average medical personnel.
Although the biomedical smart jacket is still in its prototype phase, it does seem like a breakthrough in efforts geared towards tackling a condition that doesn’t get as much attention as the usual suspects despite being quite deadly.
Although pneumonia is found to cause more death in children under five than HIV/AIDS, malaria, and diarrhea combined, it is quite baffling that schemes aimed at combating the ailment do not get significant funding with UNICEF again reporting that only two cents are directed to tackling pneumonia for every dollar expended on global health.
In view of that, Mama-Ope, which loosely translates to “Mother’s Hope,” does come across as a timely intervention, offering hope against a disease which is a bigger nightmare for children than any other.

Turybagye ingenuous efforts saw him clinch the Pitch@Palace Africa Prize in 2017. That same year, he was also named as a contender for the prestigious Royal Academy of Engineering Africa Prize.
In a country like Uganda where a shortage of qualified medical personnel continues to hamper quick and reliable healthcare service, the cutting-edge biomedical jacket could provide respite to the millions that could be affeceted in adverse ways.
Featured Image Courtesy: ehealthnews.co.za